Okay, let’s talk about “intersex genitalia”, or using its proper term, ambiguous genitalia and how sex is determined. First of all, it is not some doctor, rubbing their chin, doing a sharp intake of breath and writing down a question mark, or a “best guess”, with a shrug. This really minimises the experience that parents of intersex babies go through and the advances we have made in identifying and treating DSDs.
Before we begin, let’s address what we mean by ambiguous genitalia. Many people think we mean genitalia that cannot be categorised as male or female at all. This is a common misconception. What we’re actually talking about is genitalia that cannot be easily classified as male or female upon initial observation. I’ve written about ambiguous genitalia in genetic females and genetic males who are born with female genitalia before, but here’s a quick summary from an alternative source (I’ll post the most relevant bits), with some additional information about other forms of male ambiguous genitalia:
Babies who are genetically female (46 XX DSDs) may have:
- An enlarged clitoris, which may resemble a penis
- Closed labia, or labia which include folds and resembles a scrotum
- Lumps that feel like testes in the fused labia
Babies who are genetically male (46 XY DSD) may have:
- Hypospadias – when the urethra doesn’t fully extend to the tip of the penis
- An abnormally small penis with the urethral opening closer to the scrotum
- The absence of one or both testicles in what appears to be the scrotum
- Undescended testicles and an empty scrotum that has the appearance of a labia with or without a micropenis
One of the conditions that can cause ambiguous genitalia is congenital adrenal hyperplasia (CAH). In the case of salt-wasting CAH (one of the two forms of classic CAH), this can be fatal for babies if left undiagnosed. This of course must be monitored. So, when a midwife sees ambiguous genitalia, a whole raft of experts become involved. This includes, but is not limited to, specialists from endocrinology (hormones), urology/gynaecology (kidneys, bladders, genitals) and psychology. Other team members may include nurses, geneticists, neonatologists, and people who work in the labs. Some smaller hospitals may not have these specialist teams, so the baby may need to be moved to a larger hospital that can offer the required services in one place.
These specialists will carry out a number of investigations and tests. Doctors examine the baby and ask about their family’s medical history. They also check the baby’s chromosome pattern with a blood test. The chromosome pattern (aka karyotype) helps doctors understand the background to the child’s development and consider which direction to take the further tests. The initial karyotype result usually takes 2-3 working days to come back. That’s a long time for a new parent.
Many babies are kept in hospital for the first few days so that salt levels in the blood can be monitored. Doctors will also measure hormone levels in the blood, and possibly in the urine, to see how the adrenal glands and gonads are working. Ultrasound tests and scans can sometimes show the internal sex organs (such as the womb/uterus). Again, these are best performed in specialist centres and can sometimes be difficult to interpret. Doctors take their time; they do not shrug and guess. Doctors might rarely look at the bladder and opening of the vagina with a special cystoscope and very rarely they might look at the gonads with a laparoscope and examine tissue samples (biopsies) from them. All of this may be part of the diagnostic process.
Once sex is determined, the doctors’ involvement does not end there. If response to hormones has been flagged as an issue, medical interventions will also be necessary to help the child through puberty. It’s not a “fun talking point” or just some quirky variety in genitals that causes doctors to throw all medicine and science out of the window. The parent may have to make choices about surgical interventions etc. I’ve included a couple of tables at the end of this post that expand on some of the DSDs which may present with ambiguous genitalia and the possible interventions that may occur.
All of this at a time when parents are normally celebrating their new arrival. This brilliant booklet from dsdfamilies really hammered home to me how much additional support parents of a new-born intersex baby needs and how different their experience is. I really would recommend reading the whole booklet if you would like to learn more.
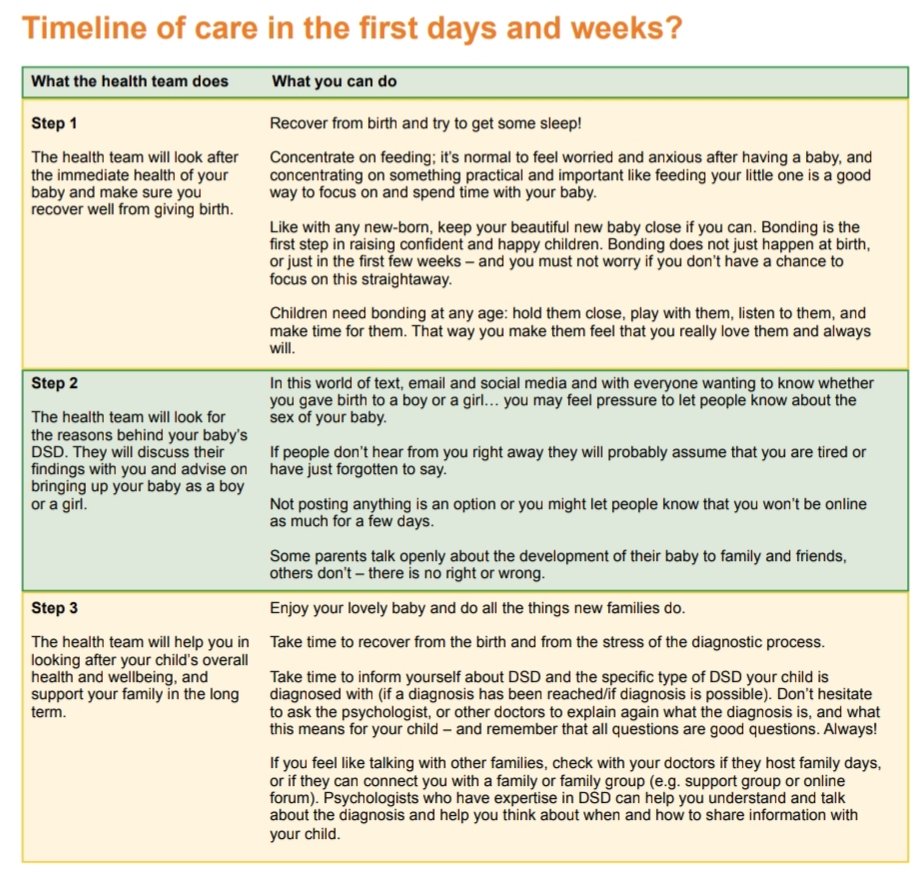
You can also read more about the various DSDs that may result in ambiguous genitalia, the diagnostic process and any treatment that may be needed immediately after birth and throughout the persons lifetime in this clinical guide from the BMJ.

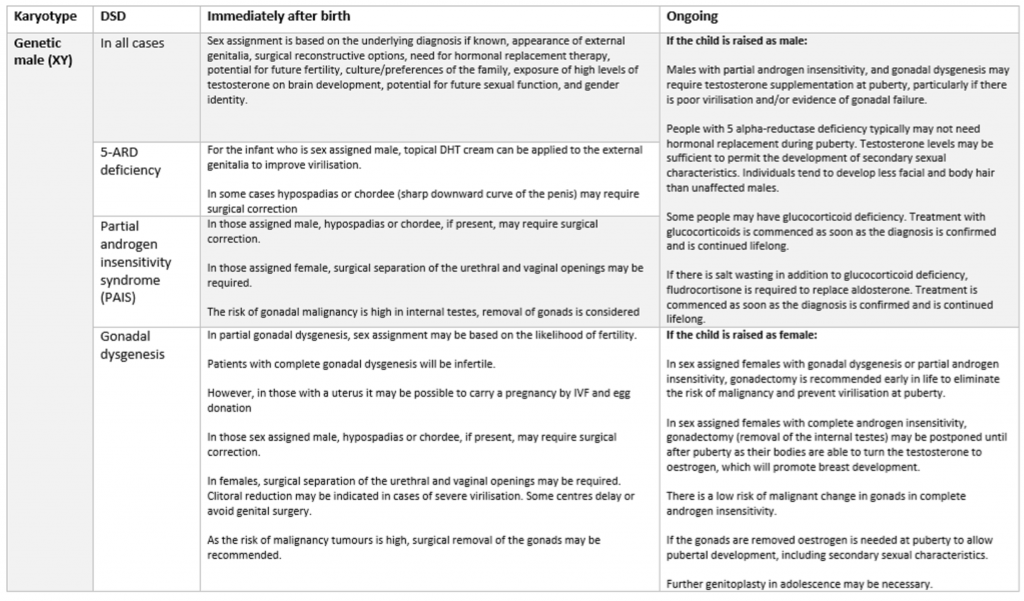
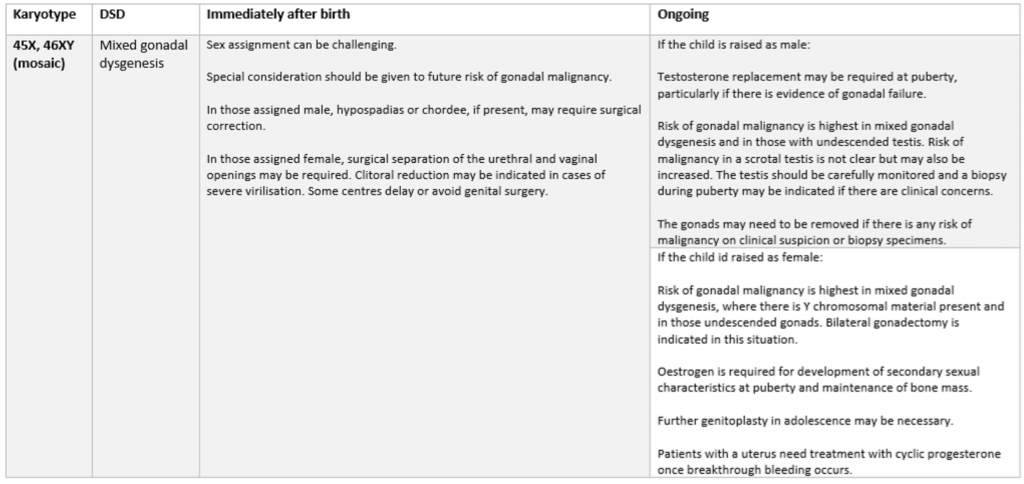

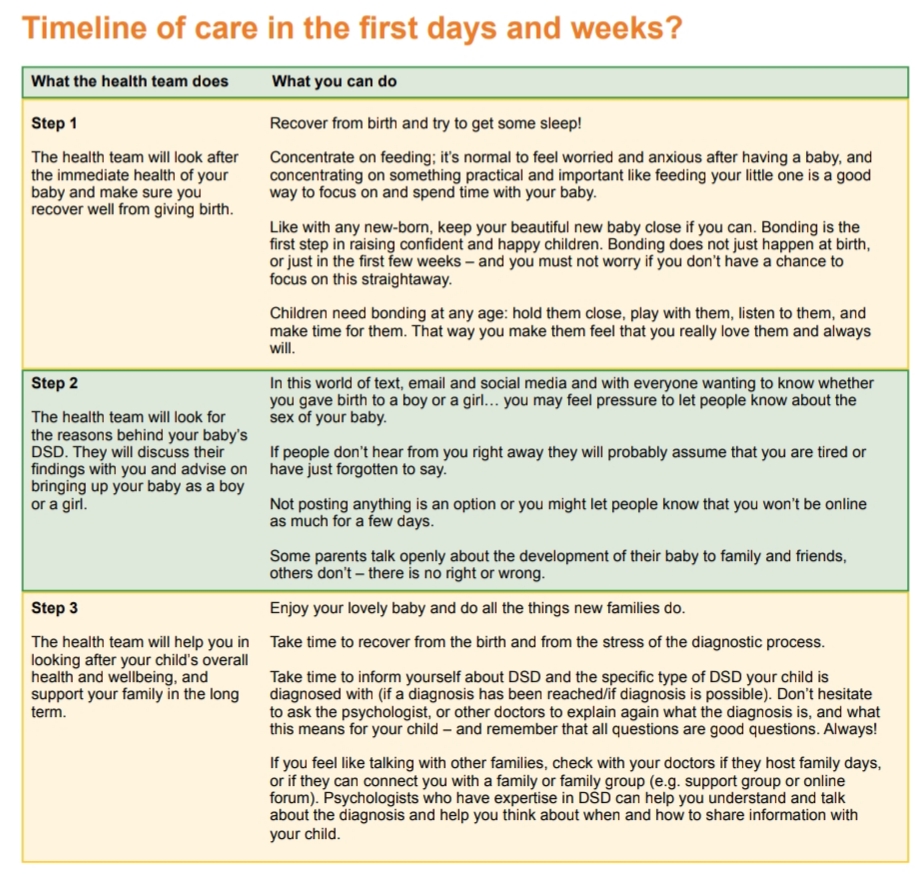
Interesting piece, but you don’t answer your title question: is there such a thing as “intersex genitalia”?
Depending on definitions, the answer can be: yes.
For example, it’s clear in many case-studies (which include photo-evidence) that intersex-births (and continuing through to later life as adults), can have both a ‘penis’ and a ‘vagina’ which presumably can rightly be labelled ‘intersex genitalia’ aka ‘ambiguous genitalia’.
But some forms of genital-combination are not possible due to the either/or nature of bi-potential tissues in early fetal-development
i.e. can’t have both a clitoris and a penis, nor can a baby have both a scrotum and labia.
I’m not sure you really read this properly. At the beginning, I describe what ambiguous genitalia actually means. In short, underdeveloped male genitalia or virilised female genitalia, never a mix of both. Someone with “a penis and a vagina” would actually be either a female with a enlarged clitoris and a vagina, or a male with a penis and underdeveloped scrotum which appears like a vagina, but is not one.
But that’s my point – your title refers to ‘intersex genitalia’, but then you never use that phrase anywhere in the article.
It’s not clear if your use of ‘ambiguous genitalia’ means the same thing, so you don’t ever answer the question: is there such a thing as “intersex genitalia”?
Not sure there’s a clear distinction between ‘an enlarged clitoris’ and ‘a micropenis’ as both are developments of the same bi-potential tissue, and are ultimately named one or the other in the context of the biology/genetics of the baby.
I think it would be helpful to define ‘intersex genitalia’ as it could be argued this is a valid name for the genitalia of CAIS individuals i.e. female typical (clitoris and vagina) but not a full vagina (no upper-barrel, no uterus etc.) and the baby is karyotype 46XY?
You seem to be moving the goal posts now. As CAIS genitalia is unambiguously female, I’ve never seen anyone refer to it as “intersex genitalia”. By that token, a girl with MRKH’s underdeveloped vagina is also “intersex genitalia”, as would be the unambiguous penis on a man with Klinefelters. Most people when they use the term use it just like you did, to mean a mix of both. In those cases, what they are actually referring to is ambiguous genitalia.
In the absence of you defining what ‘intersex genitalia’ means, I was making the point that it could be argued that it refers to the genitalia of any intersex person i.e. CAIS and PAIS is intersex, so whether the genitalia are fully female or partially, they’re both intersex.
As per Leornard Sax’s definitions and pushback on Fausto-Sterling’s 1.7% claim, Klinefelter is never intersex i.e. there’s nothing ambiguous about the genitalia, and no mismatch between phenotype and genotype.
To clarify, are you saying ‘intersex genitalia’ and ‘ambiguous genitalia’ means the same thing, and that the answer to the title of your piece is: yes?
No, as there is really no such thing as any genitalia that cannot be classified as a penis or a vagina. That’s the point. People talk about male, female and intersex. Penises are male, vaginas are female. This applies to all intersex cases too, even cases of ambiguous genitalia.
I’d also add, I’m not into narrowing the definition of intersex to exclude people who rely on the community for support. The problem is the word “intersex” and what people, like yourself, think it means. This is why differences of sex development (DSD) is actually are more accurate term, but I also know this is contentious and is not a term everyone recognises.
I don’t think we should allow the expansion of the definition of intersex for ulterior reasons. Sax gives it a clear and unambiguous definition that reduces the 1.7% claim to 0.02%
Men with Klinefelter syndrome should get all the support then need, medical and otherwise, without having to be incorrectly included in a category that does not apply.
Well, it’s not up to you, so we don’t need to worry about that, do we? Good to know there are still people out there whose main priority in life is excluding people from the support they need. Intersex, put simply, is an umbrella term for a variety of different conditions that affect the development of the reproductive tract. That’s all. You want it to mean “in between”, it doesn’t. It never has. Scientifically, it was coined to describe how different factors interplay in reproductive development. The politicisation of the word, as you are doing, helps no one. Least of all people with DSDs.
Ok, then I have no idea what you mean.
Clearly an individual can be born with a penis and vagina & labia, the very definition of ambiguous genitalia, which could or could not also be called ‘intersex genitalia’ if you bothered to define what you mean by that term (if you don’t want to define/clarify it, why use it in your article-title, and then ignore it completely in the text of your piece?)
Only on further investigation (scans, genetics, endocrinology) could we establish the wider context of the (clearly) intersex condition, and conclude the biology/genetics etc. and then maybe redefine genitalia as enlarged-clitoris or micro-penis etc.
Yeah, you’ve missed the point entirely. No one can be born with a penis and a vagina. I’ve already explained this to you. It seems to me you’re just here to sealion and waste people’s time.
How miserable of you.
And how stupid to pose a question as the title of a piece, then never refer to it again.
I think it’s you who’s wasted my time. Do better.
P.S. there are plenty of experts who counter your argument about penis/vagina, but it comes down to clear definitions, something you don’t bother with.
You didn’t have to read it, bud. I’m sorry you didn’t get to rewrite my blog for me. Why not write your own? As for experts, you seem to have also missed the link to the BMJ there. Are you sure you even read this?
A baby is born with ambiguous genitalia, small-penis and vaginal/labia. Or is it enlarged clitoris and vagina/labia? Further investigation.
Discover baby is 46XY with PAIS, so small-penis.
What do you now call the vagina/labia? Not a scrotum. And despite being shallow, missing upper-portion and no cervix/uterus, what do you now call the opening and folds that are clearly vagina/labia like?
Again, no one is born with a penis and a labia. What is it that you cannot accept about this? Find me one science/medical paper that makes this claim. I can wait.
To answer your question about the baby with PAIS, if it’s discovered that they have a penis, then they also have a scrotum. In cases like this the scrotum is underdeveloped, so the skin folds appear like a labia, but they are not. As I say, I clearly explained this in the blog you don’t seem to have read, but are arguing over anyway.
Claire, why not just cut the snark out, ok?
Of course I’ve read your piece, a number of times.
And I’ve taken the time to (politely) ask why you haven’t answered the question you pose in the title, nor even use the title-term ‘intersex genitalia’ anywhere in the article – questions you still haven’t answered.
As for ‘ambiguous mix of genital characteristics’, it seems you’re determined to label all features depending on the biological sex of the baby i.e. genitals MUST be exclusively male or female, irrespective of how each feature has developed and appears under observation.
We know a new-born can NOT have both a penis and clitoris, nor can they have both labia and scrotum. Because the penis and the clitoris are the same organ developmentally, thus you can only have a penis OR a clitoris; similarly, the labia and the scrotum are the same organ, developmentally.
But in rare-circumstances (e.g. AIS and CAH) genitals do not develop along clear male or female lines, and it can be a complicated mix.
I get it you want to redefine what may look like labia as a scrotum once we discover a baby is 46XY. But I don’t understand why you can’t accept that, given the clitoris/penis develops out of one bi-potential organ/tissue, and the scrotum/labia develops out of another separate independent bi-potential organ/tissue, you can’t have a mix?
I don’t have access to scientific-papers, but I can point to a short piece by Alice Dreger, someone I’ve followed and admire (if you haven’t read ‘Galileo’s Middle Finger’ I highly recommend it).
Alice’s piece (http://alicedreger.com/both_sets_of_genitals) includes this:
“The person was born with a phallus too large to look like a typical clitoris plus a vaginal opening. That is possible with various conditions, including partial androgen insensitivity syndrome, and 46,XX CAH; see figures 3 and 4 here for an idea of what it can look like when you have a noticeable phallus and a vaginal opening. (So why isn’t that “both sets of genitals”? Um, because the person doesn’t have both a penis and a clitoris, both labia majora and a scrotum, etc. There’s a LOT more to genitals than just penises and vaginas, people! Just having a big phallus and a vaginal opening doesn’t give you two sets of genitals.)”
Males do not have anything akin to a vaginal-opening, there’s nothing about a scrotum that would suggest that’s what this is. So, it’s a vagina – what else can it be?
If we play with words/definitions as you seem determined to do, wouldn’t we have to say that a person with CAIS (i.e. genitals totally indistinguishable from ‘normal’ female genitals) actually has an underdeveloped-penis and underdeveloped-scrotum?
Do you feel you have the right to tell a CAIS individual that, someone who insists they have female genitals, and that they are female?
In the same way that you want to tell a Klinefelter individual he’s intersex, even if he objects to being labelled by you?
You do realise that Alex Dreger quote agrees with me and not you, yeah? Understanding what the body parts are is important for giving a person born with ambiguous genitalia options for corrective surgery, should they want it later in life. It’s really offensive of you to keep suggesting an underdeveloped scrotum is a vagina, but I get the impression you don’t care about that. If you did, you wouldn’t be here spreading disinformation by stigmatising males with DSDs. And, no, as person with CAIS has female genitalia they do not have an underdeveloped penis and scrotum, they have a clitoris and vagina. This isn’t playing with definitions, it’s scientific fact and I’m sorry the reality of ambiguous genitalia makes you so uncomfortable you can’t accept it for what it is. This is the reason IGM exists. You do you though.
Btw, I’ll be as snarky as I like at trans activists who stigmatise intersex people and spread harmful misinformation that props up structural violence. You should stop fetishising intersex people and work on accepting yourself.
Oh, and no one is telling men with Klinefelters that they have to use the label intersex. In fact, I’ve clearly said to you I would get rid of the label all together as the politicisation of the word by non-intersex people has done us no favours, which really shows that you don’t actually read anything (no suprise given you used PAIS as an example which was clearly explained on the BMJ site). That said, people use the label, including men with Klinefelters, and I support that. It’s you that wants to dictate that those who are counted shouldn’t be. Mainly because you want to believe in hermaphrodites, which, btw, no intersex orgs agree with. And certainly no woman with CAIS would welcome the inaccurate bs you’ve just said about their genitals.
Consider two cases of new-borns.
Case 1:
1 – Karyotype 46XY
2 – Internal testes producing ‘normal male levels’ of testosterone
3 – No ovaries, no womb, no residual Mullerian duct
4 – Vaginal-opening with labia, both indistinguishable from ‘normal’ female
5 – Vaginal-depth only 2/3rds of ‘normal’ female (as upper 1/3rd is created from Mullerian duct)
6 – Clitoris indistinguishable from ‘normal’ female in position, form, and size
7 – Urethra-opening positioned between vaginal-opening and clitoris, as with ‘normal’ female
8 – This is a CAIS individual i.e. unambiguous female genitalia despite male genotype and male gonads
Case 2:
1 – Identical to points 1 thru 5 in case 1
2 – Has a penis indistinguishable in position and form from ‘normal’ male (i.e. skin-covered shaft, glans covered by foreskin etc) but slightly smaller than average
3 – Urethra-tube runs through middle of penis, opens at tip of penis
4 – This is a PAIS individual i.e. ambiguous genitalia despite male genotype and male gonads
Given the ‘vagina/labia’ are identical in both cases, why is it NOT a vagina in case 2?
Yeah, you making up cases doesn’t change reality, does it? We’ve been over this. You are incorrect. Get over it and, as I say, stop fetishising babies genitalia. It’s not a good look. K?
Prove case 2 PAIS doesn’t exist?
Clearly you’re blindsided by your own corrupt motivated-reasoning.
Disappointing you display, in spades, the crass juvenile name-calling you criticise Twitter for.
Read ‘Galileo’s Middle Finger’, and reflect on the crap Alice Dreger had to put up with from folk like you.
Truly a miserable dishonest bad-actor when we need honest debate about these issues.
Lol…It’s up to you to prove it does exits, bud. That’s how science works. I’ve explained what ambiguous genitalia is. I’ve linked to a respected source, in fact more than one, that agrees with me. It even mentions the condition you’re trying to claim. I’m sorry this hasn’t worked out for you. I’m not the one with a corrrupt motivation. Your DARVO won’t work here either. People have a right not to touch your penis if they don’t want to. I suggest you get some counselling to deal with that instead of making up fictitious intersex conditions to “justify” your fetish.
It’s interesting how so many in the Trans try to say their is such thing as Intersex genitalia but they can’t seem to prove it. The only thing remotely close is Ambiguous genitalia and most Intersex conditions have Ambiguous genitalia and it all depends upon genetics, DNA and Karyotype. In my Case, I have Kallmann’s syndrome in the Kal-1 gene and in that variation, I have Ambiguous genitalia and a micropenis.
Hi Nicky, nice to meet you and thank you for sharing your story. I think there’s so much taboo around this that many people feel too ashamed or stigmatised. The more we talk about it, the more myths we dispell.
The more people know that their are Intersex/DSD people like myself that exist, the more we dispel the myths that the Trans like to pull onto people. I have seen way too many trans who try to claim to be Intersex and can’t even prove with Biology and medical science. It’s why the Trans are scared of people like me because Intersex/DSD people like myself have disproved their theories and myths about intersex/DSD people
I know exactly what you mean. I used to have a Twitter account where I wrote about my own DSD and shared information about others. I was harassed and bullied by trans activists to try to get me to stop. When that didn’t work, they organised mass reporting of my account until Twitter banned me. It spurred me on to write the blog though, so it still didn’t achieve what they wanted. I’m glad to see others becoming more vocal too.
It happened to me too and it’s why I am no longer on Twitter. Instead, I am on Gab, Mewe, Minds, Bitchute and Parler. I was bullied out by the Trans activist because they tried to silence me for exposing them and trying to tell my Intersex/DSD story. Lucky my story is still online and many of them can’t even attack it and this is the one
What It’s Like to Be an Intersex Nudist
https://www.thecut.com/2015/09/what-its-like-to-be-an-intersex-nudist.html
Oh wow….your story is fascinating. Thank you again for sharing it. I’m sorry you’ve also had a shit time with trans activists. Hoepfully we will reclaim our own advocacy again.
I’m hoping that twitter cleans it’s act up but I’m not holding my breath because the Trans have a stranglehold on Twitter. My Intersex story is why I exist and my Intersex/DSD condition.
Thank you for this great blog, Claire, and thank you Nicky for your brilliant article. I’m trying to help educate TRAs who are misusing the term ‘intersex’ and it’s so illuminating to read your stories. I will share them all over Twitter!
Claire…… you have gone from my Twitter feed… I have been off twitter for a short while. What happened?
I got banned again. I’ve appealed but not had much joy tbh. It’s really frustrating.
Hi Claire, I have some thoughts:
I think that you are doing a disservice to other intersex people by saying that you can always refer to their genitals using allosex terms. Scrotum, micropenis, labia, clitoris etc. The fact is that the tissue involved in the development of these structures is the same, and we start with the ability to develop either. Saying that someone whose glans developed slightly towards the male pole (Heh, pun not intended.) has a micropenis isn’t really correct, and doesn’t really accurately describe the phenotypic reality of the person, and isn’t really helpful.
I’d also like to note that you’re seeming to support the mutilation of other intersex people, such as myself, by posting the diagnostic and treatment criteria recommended by the very people who perform those mutilations. Is this because you’ve been swept up by their rhetoric that they just want the best for the child? If that were true, “It’s easier to dig a hole than build a pole” wouldn’t still be in common parlance among their ranks. My parents were manipulated into allowing the doctors to mutilate me, plain and simple. The same is still done to this day, decades later.
The fact is that they are penises and vaginas though. I’d say it’s more of a disservice to deceive people with DSDs, as was done in the past.
I’m not sure where you’re getting “support for mutialtion” from either, other than you seem to be attributing things to me and the sources I’ve shared that actually aren’t contained within them. This would suggest that it’s maybe you that’s swept up in the rhetoric here.
No, the fact is that it is much more complex than you’re making it out to be, with a very important grey area between.
And please, read your own sources. The BMJ says that clitoral mutilation may be needed if it’s too big under XX patients. It’s literally right there. Do you even understand what those of us who are mutilated go through and what *we* want? Or do you only talk to anti trans dyadic people?
It really isn’t more complex. It’s a shame you want to lie to Intersex people about their genitalia. How do you think that will help parents to make informed decisions, exactly? We actually know that perceptions of uncertainty and the stigma surrounding that are one of the key factors that makes parents feel forced to consent to unnecessary surgeries.
The BMJ does not promote mutialtion, as you keep trying to claim. As you say it actually states surgery *may* be necessary. Sometimes surgery is. Denying this is not helpful for people who may have a different experience to yours.
Surgery on the clit or glans of a female appearing Intersex person is *never* needed. Period. That graphic says it may be needed if the glans or clit is too big for a female appearing person.
You need to learn from people who were mutilated, instead of trying to talk over us.
I’m not talking over anyone. You’re here commenting, pretending your experience is the only one available and promoting intersex people being lied to. That’s a very odd stance for an IGM victim to take, if I’m honest. Most would support accurate information and be against concealment. Why do you want intersex children’s experience to mirror yours if you disagree with it? Your stance makes zero sense.
Alright, let’s hold on a second, since you’re accusing me of wanting to lie to other Intersex people:
At what point does the bipotential tissue that can develop into the penis or the clitoris become, in your opinion, a penis, and at what point does it become a clitoris? The same question applies to the scrotum and labia. It should be easy to answer this question, if your view is correct.
You should read the rest of my blog. I answer all of these questions.
Point me to it, then. I’ll read there and reply on that post.
You can click on the homepage and look through it yourself. Given how rude you’re being, I’m not sure why you expect me to even do that for you. If you can’t be bothered, I suggest you take your anger elsewhere.
Hi Claire,
I hope you are well – it’s been a while since I have dropped by and have been catching up with your articles.
I have left you a beer or two behind the bar 🙂
https://www.paypal.me/mrkhclaire
(That’s a hint to anyone else passing by this way)
Best wishes xx